Your path to clear skin starts here.
Skin care from an acne expert.
Specialty ACOM Prescriptions
Specialized Acne Care for Skin of Color
You deserve a clear complexion.
Acne in Skin of Color
Adult Female Acne
A center dedicated to acne.
Learn More about Adult Female AcneAcne Center of Michigan
We are your experts for acne and acne scarring
Our Mission
We strive to provide the best acne skin care treatment in Metro Detroit. Our mission is to offer a comprehensive acne treatment plan, drawing from both traditional and alternative approaches. Dr. Singer will work with each patient to understand, educate, and achieve the goal of a clear complexion.
Acne Treatment Gallery
Want to see some of our patients’ results? We have a gallery of several treatment before-and-after photos & videos to show you examples of the different types of acne we treat and the results of our prescribed treatments.
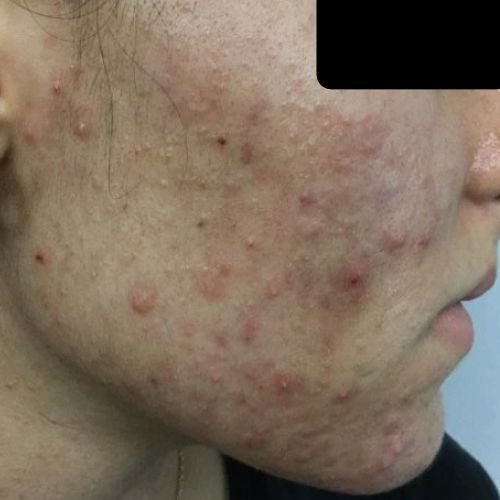

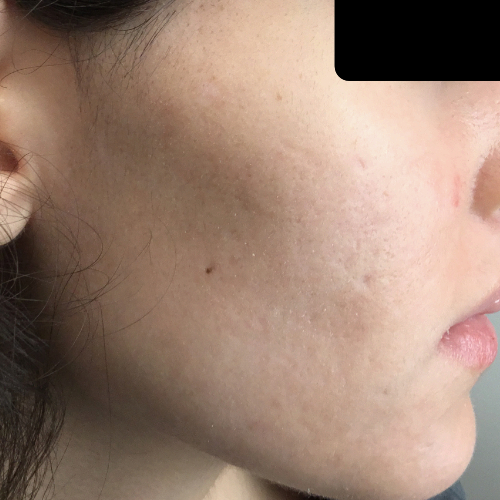




Located in Bingham Farms, Acne Center Of Michigan was founded by Dr. Craig Singer, a board-certified dermatologist.
We specialize in the treatment of acne and acne scarring, offering numerous therapeutic options tailored to each patient’s needs.
Dr. Singer experienced significant acne when he was in college and has personal experience with his teenage children’s acne as well. He has helped thousands of patients look their best.
Acne Center of Michigan offers the most advanced acne treatments, including traditional and alternative approaches.
Our mission is to give you the clear complexion you deserve.













Our Services
Traditional Treatments
Oral and topical therapies.
Chemical Peels & Light
Non-invasive therapies.
Acne Scarring
Defect-oriented therapy.
Amazing results
VIPEEL Precision plus
Purchase 2 VIPeels at full price and get the third 50% off.


Patient Testimonials






Recent Articles

Diet and Acne
You are what you eat. But, does diet cause acne? Acne is a common skin condition that affects people of all ages, and many factors

A dietary supplement can improve Acne Excoriée (skin picking in acne).
Acne excoriee is a skin condition that is often overlooked and misunderstood. It is a compulsive disorder that involves picking at acne lesions, resulting in
How to take Accutane and prevent side effects
Accutane was the original brand name of the chemical compound isotretinoin. Even though multiple preparations of isotretinoin have been formulated and are sold today through