Psoriasis
Pronounced "Suh-rahy-uh-sis"
If applicable, slightly more detailed or comma-separated list
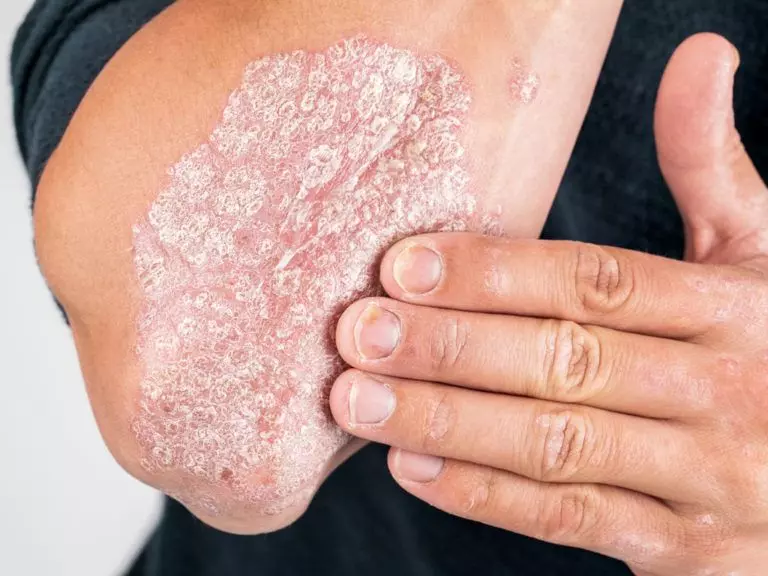
What is Psoriasis and what does it Look Like?
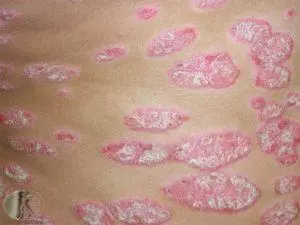
Psoriasis is chronic immune-mediated disease in which scaly, red, raised patches appear on the skin. Psoriasis usually affects the elbows, knees, and scalp though it may involve any part of the skin surface including the nails and genital region. Patches of psoriasis typically become raised (i.e. plaques) with thick white scale causing itch and discomfort. The social stigma of psoriasis may be a source of embarrassment and may lead to depression. It is important to remember that psoriasis is not contagious and you cannot “catch it” from another person. Effective treatments exist and in many cases, psoriasis is completely controllable.
The classic presentation of psoriasis consists of thick white scaly inflamed plaques (i.e raised patches) located on the outer elbows and knees with involvement of the scalp and gluteal cleft. Some people have thicker patches than others. Some have more itching than others. Less common sub types include:
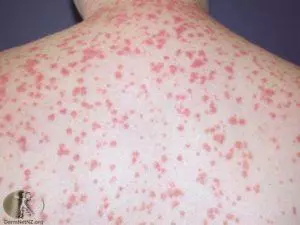
- Guttate variety (tear drop sized lesions) scattered on the trunk, arms, and legs.
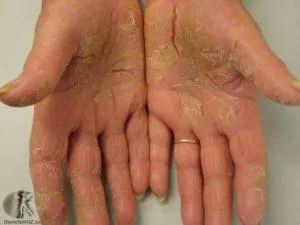
- Hand and Foot variety consisting of thick skin on the palms and soles with painful splits in the skin.
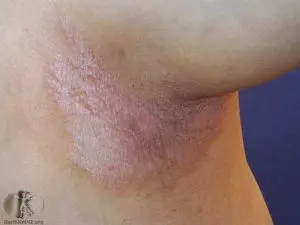
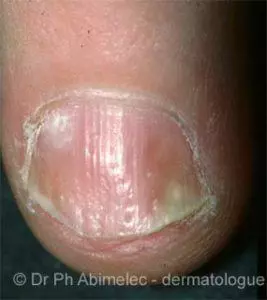
Many people also experience red patches in the genital region and some develop involvement of the fingernails and toenails. Finally, 10-15% of people with psoriasis also develop arthritis.
Photos courtesy of DermnetNZ
Frequently Asked Questions (FAQ)
We are not exactly sure why someone develops psoriasis however, we do know that genetics plays an important role. Research has shown that the immune system is overactive and causes the skin cells to grow at an abnormally fast rate. Sometimes there is an obvious trigger such as an infection with group A streptococcus or a medication such as a beta blocker. In many cases, however, the trigger is unclear. You are more likely to develop psoriasis if family members have it too. Approximately 1 in 3 people have an affected family member. On average, psoriasis affects 2-3% of the population. It usually shows up between 15-35 years of age, but can develop at any time. Up to 15% of psoriasis starts during childhood.
A number of factors influence the treatment approach to psoriasis:
Is the psoriasis localized to just a few areas on the body? Or is it widespread?
How much body surface area is involved? Greater than 10% body surface area is considered moderate to severe.
- Are the patches of psoriasis thin or thick?
- Are the patches itchy?
- Is there involvement of the hands and feet?
- Is there involvement in the genital area, groin or armpits?
- How bothered is the person about his or her psoriasis?
- Are the nails involved?
- Is there psoriatic arthritis?
- Does the person have a history of a weakened immune system? Or a history of cancer?
Treatments for Psoriasis
A number of topical therapies are available for psoriasis and are most often used for localized areas.
The most common topical therapy for psoriasis is superpotent topical steroids (e.g clobetasol, augmented betamethasone, halobetasol). Topical steroids are available in a variety of vehicles such as creams, lotions, ointments, sprays, gels and foams. Topical steroids work by reducing inflammation and restore the normal thickness of the skin. Sometimes Saran wrap is used to occlude topical steroids in order to enhance their penetration into thick plaques. Local side effects limit long-term continuous use of potent topical steroids.
Topical vitamin D preparations such as Dovonex and calcitriene are often effective in maintenance therapy of psoriasis. Some therapies combine both topical steroids and topical vitamin D into one vehicle (e.g Taclonex and Enstillar). Topical retinoids such as Tazorac may also be of effective treatment for psoriasis but these are sometimes irritating to the skin.
Topical calcineurin inhibitors such as Protopic and Elidel are non-steroidal and valuable for use on the face, axilla, groin, and genital region.
Other nonsteroidal options include ammonium lactate lotion, salicylic acid, and urea to soften the plaques. Classically, coal tar has been used in various preparations but has fallen out of favor due to the fact that it can stain clothing and is messy to use.
For thick, localized areas of psoriasis such as thick plaques on the scalp as well as on the legs, intralesional injection with triamcinilone can be quite effective. The downside is the pain and the number of injections required to properly treat each plaque. The upside however is that the plaques may remain in remission for months. This is considered a very safe treatment with minimal side effects. Typically, the small amount of intralesional steroid use does not produce any systemic side effects.
Narrowband UVB light therapy is available in an office-based light box, handheld XTRAC laser, as well as in hand and foot units. Narrowband UVB is felt to be much safer than light obtained in a tanning salon. For those patients with greater body surface area involvement and those with guttate psoriasis, narrowband UVB is extraordinarily effective in producing clearance in up to 75% of people. Risks include burning, photoaging, and potentially increased risk of non-melanoma skin cancer. Also, the treatments must be done 2 to 3 times a week for a minimum of 10 weeks, and then require ongoing maintenance therapy approximately once a week indefinitely. Some patients who respond well to narrowband UVB qualify for a home therapy unit.
Recent advances in therapeutic options has led to the expectation that all patients with psoriasis should be able to achieve substantial clearance of their psoriasis with the ultimate goal of driving down psoriasis to less than 1% body surface area.
The term “PASI 75” has become the benchmark for measuring treatment success in psoriasis. If one achieves a PASI 75, it means there is a 75% improvement of psoriasis from baseline.
The entire skin surface encompasses 100% body surface area. The size of the adult palm represents approximately 1% body surface area. So if the entire scalp is covered with psoriasis, this would constitute 10% body surface area. If half of the trunk is involved, this would constitute 18% body surface area, and so on.
A person with 5% to 10% body surface area is considered to have moderate psoriasis.
A person with more than 10% body surface area is considered to have severe psoriasis.
Once a person has more than 5% body surface area, it starts to become impractical to treat all sites with topical therapy alone.
Systemic therapy is indicated for patients with moderate to severe psoriasis, for those with psoriatic arthritis, and in patients who are unresponsive to other forms of therapy. Systemic therapies generally work by modulating the immune response. Systemic treatments may be given orally or by injection.
Otezla (apremilast) was FDA approved in 2014 for the treatment of moderate to severe plaque psoriasis and psoriatic arthritis. It is typically dosed at 30 mg twice daily. Clinical trials indicate that approximately 31% of patients taking Otezla achieve a PASI 75 score after 16 weeks of therapy. Otezla works by inhibiting phosphodiesterase-4 which reduces levels of TNF– alpha and IL–23, inflammatory mediators of psoriasis. The most common side effect is diarrhea. Fortunately most gastrointestinal side effects improve after one month of therapy. Unlike biological agents, there is no increased risk of opportunistic infection or lymphoma. In addition there is no laboratory monitoring. Some insurance companies will not approve Otezla until the patient has failed biological therapy first.
Otezla fact sheet
Soriatane (Acitretin) is a retinoid medication that normalizes skin proliferation. Soriatane thins out plaques of psoriasis making topical medications and phototherapy more effective. Previous studies indicate a 34% PASI 75 at 12 weeks of treatment. Soriatane is considered a first-line therapy for uncommon forms of psoriasis such as pustular and erythrodermic subtypes. Common side effects include dry lips and skin, joint aches, hair loss, sensitivity in the sun, as well as elevation of liver enzymes and cholesterol. In addition, Soriatane should never be used in women of childbearing potential. Soriatane does not increase the risk for infection or cancer.
Soriatane fact sheet
Methotrexate has been used for psoriasis since the 1970s. Methotrexate inhibits an enzyme inside of white blood cells called dihydrofolic acid reductase, causing reduced levels of T cells in the blood. After 16 weeks of treatment, 41% of patients experience a PASI 75. The major issue with this medication is the number of potential side effects including abnormalities of the bone marrow, liver and lungs. Patients with a history of liver disease, regular alcohol consumption, high cholesterol or obesity are at higher risk of liver disease from methotrexate. Also methotrexate is contraindicated during pregnancy.
Methotrexate fact sheet
Cyclosporine is an immunosuppressive medication originally developed for organ transplant patients. Due to the potential toxicity, it is only used in extreme circumstances for short periods of time. It is not a long-term therapy.
TNF-alpha inhibitors are the first class of biological therapies introduced for the treatment of psoriasis and psoriatic arthritis. TNF-alpha causes inflammation and proliferation of the epidermis and high levels of TNF-alpha are present in the skin and joints of patients with psoriasis. Side effects of TNF-alpha inhibitors include higher rates of upper respiratory infections, injection site reactions, worsening of pre-existing congestive heart failure, reactivation of tuberculosis, worsening of hepatitis B and multiple sclerosis, and potential increased risk for lymphoma and opportunistic infections. Some patients who have had good success with TNF alpha inhibitors may notice loss of efficacy and recurrence of psoriasis over time (AKA “biological fatigue”). TNF alpha inhibitors have been shown to have additional positive benefits including reducing the risk of heart attack.
Enbrel is a fusion protein that blocks TNF alpha through competitive inhibition. It is dosed at 50 mg a week by the patient after being initially given at 50 mg twice a week for the first 12 weeks. Approximately 50% of patients achieve a PASI 75 after 12 weeks of therapy.
Enbrel fact sheet
Humira is a monoclonal antibody to TNF alpha. It is dosed at 40 mg every other week by the patient. Approximately 70% of patients achieve a PASI 75 after 12 weeks of therapy.
Humira fact sheet
Remicade (infliximab) is a chimeric monoclonal antibody given by intravenous infusion typically every eight weeks after initial loading doses. In clinical trials, 80% of patients on Remicade achieve a PASI 75 at 10 weeks.
Remicade fact sheet
IL-12/23 inhibitors influence a particular pathway in the immune system (TH17) shown to be integral to the inflammation seen in psoriasis. Several genes linked to psoriasis are IL-23 genes.
Stelara was the first inhibitor of this class approved in 2009 for the treatment of moderate to severe psoriasis. In 2013, it was approved for psoriatic arthritis. It is administered every 12 weeks after initial loading doses. Approximately 70% of patients staking Stelara achieved a PASI 75 after 12 weeks of treatment. Side effects of Stelara are very uncommon but may include increase upper respiratory tract infections. Patient staking Stelara may have, in theory, an increased risk of malignancy and infection. Thus far however, the available data show no increased risk for invasive infections or malignancy.
Stelara fact sheet
Tremfya is the first released IL-23 inhibitor for psoriasis. It was approved in 2017, with very impressive PASI 75 scores around 90% at four months of treatment. Thus far, it is showing good safety profile.
Tremfya fact sheet
IL-17 inhibitors are at the forefront of psoriasis treatment. These biological agents are human monoclonal antibodies that act against IL-17A, and inflammatory mediator involved in psoriasis. By neutralizing IL-17, inflammation and thickening of the skin are prevented. Side effects that can occur with all IL-17 inhibitors include increased risk of upper respiratory infections, and thrush (candida in the mouth). These side effects can usually be managed by topical treatment without stopping the medications. A rare side effect is exacerbation of inflammatory bowel disease or possibly triggering it. In studies, patients with Crohn’s disease who were treated with IL-17 inhibitors did worse than those on placebo. IL-17A inhibitors also in theory have an increased risk for malignancy and invasive infection.
Cosentyx, the first IL-17A inhibitor was approved by the FDA in January 2015 for moderate to severe plaque psoriasis and in 2016 for psoriatic arthritis. It is dosed at 300 mg every four weeks after the loading dose. Cosentyx shows an impressive 82% PASI 75.
Cosentyx fact sheet
Taltz was the second IL-17A inhibitor approved by the FDA (March 2016) for moderate to severe plaque psoriasis. After loading doses, it is administered 80 mg per month. Clinical trials showed PASI 75 of nearly 90%.
Taltz fact sheet
The NSF offers information on: Alternatives to traditional medicine may sometimes be helpful in managing psoriasis. The National Psoriasis Foundation is the most reputable organization to offer information about traditional and complementary/alternative treatments.
No matter which therapy is chosen, it is important to remember that psoriasis is a chronic condition and that there is no cure. Fortunately, outstanding therapies exist to thoroughly control the disease.
Sources
- Supplement to The Dermatologist, Special Issue: Psoriasis Treatment Today July 2017, pages 11-37
- www.DermnetNZ.org
- National Psoriasis Foundation – www.psoriasis.org